Trusted by Practices. Proven by Results.
Medical Billing Services that Recover the 12% You're Losing to Denials
Your practice is losing 8–12% of gross collections to preventable denials while your billing vendor emails a PDF once a month. That leakage delays hiring, equipment upgrades, and provider bonuses quarter after quarter. Mediflows runs a 30-day denial audit, posts every claim to a live dashboard, and charges a flat fee never a percentage of your revenue.

Accurate Billing
Compliacne Assured
Maximum Reimbursements
Dedicated Support
WELCOME TO MEDIFLOWS
Streamlining Healthcare’s Financial Health
Get Appointment
Call US:
Email Our Team
Email us at
Get Quote Now

Precision in Revenue, Peace of Mind for Your Practice.
At Mediflows, we are dedicated to optimizing your financial health with accuracy, innovation, and integrity. We partner with healthcare providers to streamline revenue cycles, ensure maximum reimbursement, and eliminate billing burdens.
Have a look on our amazing medical services
Revenue Cycle Management
Additional Medical Services
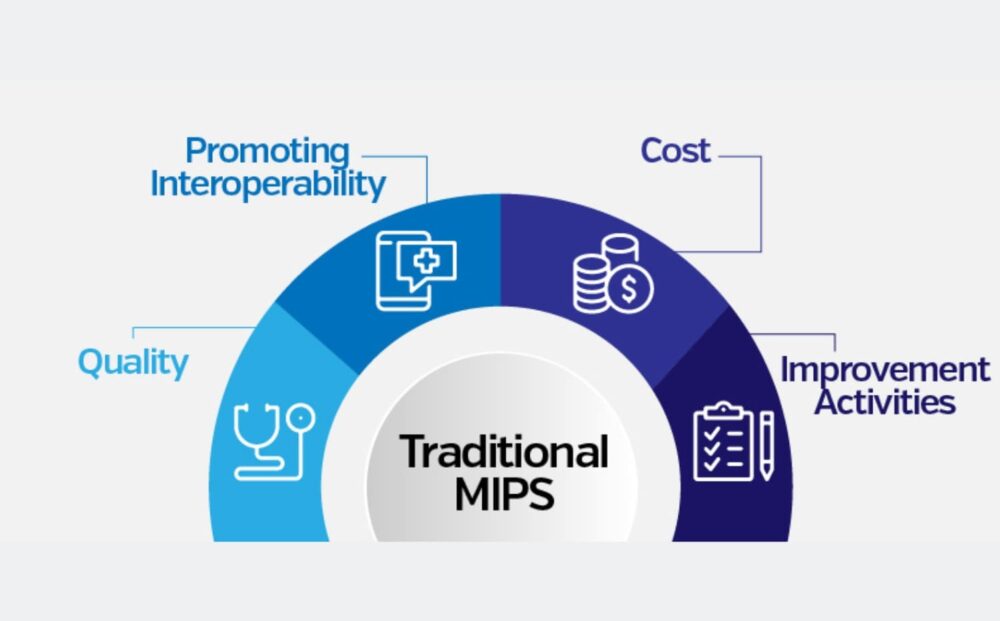
Quality Payment Program
Credentialing & Enrollment
Medical Billing
Remote Patient Monitoring

Our scale and reach to client Satisfaction
The reasons to choose Mediflows Billing Solutions
Kickoff & Access Review
30-Day Denial Audit Delivered
Clean-Claim Protocol Activated
Live Dashboard Goes Live

At Mediflows, we are dedicated to delivering exceptional billing support with compassion, innovation, and integrity. For over 20 years, we have been a offering comprehensive medical services in USA.
Billing, credentialing, and RCM tips from industry specialists
Modern AI-driven tools for faster, smarter revenue cycle mastery.
Get Quote Now
By submitting this form you are agreeing to our Privacy Policy,
We guarantee not to disclose your information.
Medical Billing FAQ
How much do medical billing services cost?
Medical billing services typically cost between 4% and 10% of collected revenue, depending on the size of the practice, specialty, and services included. Some providers may also charge flat monthly fees or per-claim pricing based on your billing volume and requirements.
What is a good clean-claim rate in 2026?
A good clean-claim rate in 2026 is typically 95% or higher. High-performing medical practices and billing teams often maintain a first-pass acceptance rate between 95% and 99%, helping reduce denials, speed up reimbursements, and improve cash flow. (breezybilling.com)
Is percentage billing or flat-fee billing better for a small practice?
For most small practices, percentage-based billing is usually the better option because the billing company only gets paid when the practice gets paid, which helps reduce upfront costs. Flat-fee billing can be more cost-effective for larger or high-volume practices with predictable claim numbers and steady revenue.
How long does it take to transition from in-house billing to Mediflows?
Transitioning from in-house billing to MediFlows typically takes between 2 and 6 weeks, depending on your practice size, EHR system, payer enrollments, and the complexity of your existing billing workflow. Our onboarding team works closely with your staff to ensure a smooth transition with minimal disruption to operations.
Do you handle credentialing and enrollment with insurance payers?
Yes, we assist with provider credentialing and payer enrollment to help ensure your practice is properly registered with insurance companies and ready to submit claims without delays.
Which practice management systems and electronic health record systems do you integrate with?
We integrate with a wide range of popular practice management and EHR systems, helping streamline billing, reporting, and workflow processes for your practice.
What specialties do you cover?
We support a variety of medical specialties, including primary care, internal medicine, cardiology, pediatrics, orthopedics, mental health, and more.
How do you handle denied claims?
Our team reviews denied claims promptly, identifies the root cause, corrects any issues, and resubmits claims quickly to maximize reimbursements and reduce revenue loss.
Are you Health Insurance Portability and AccountabilityAct (HIPAA) compliant?
Yes, we follow strict HIPAA compliance standards and use secure systems and processes to protect patient information and maintain data confidentiality.
Do I sign a long-term contract?
No, we offer flexible service agreements designed to fit your practice’s needs without locking you into long-term commitments.